Written by Professor Ian Roberts, Professor of Epidemiology at LSHTM and co-lead of the WOMAN-2 Trial.
Access to quality health services is a basic human right. This is reflected in the theme of this year’s World Health Day (7 April), “my health, my right”.
Globally, many groups are not able to access their right to health: this could be due to their gender, ethnicity or social and economic status. It could also be due to a lack of trained healthcare professionals, the inaccessibility of medication and equipment, or the scarcity of public health information.
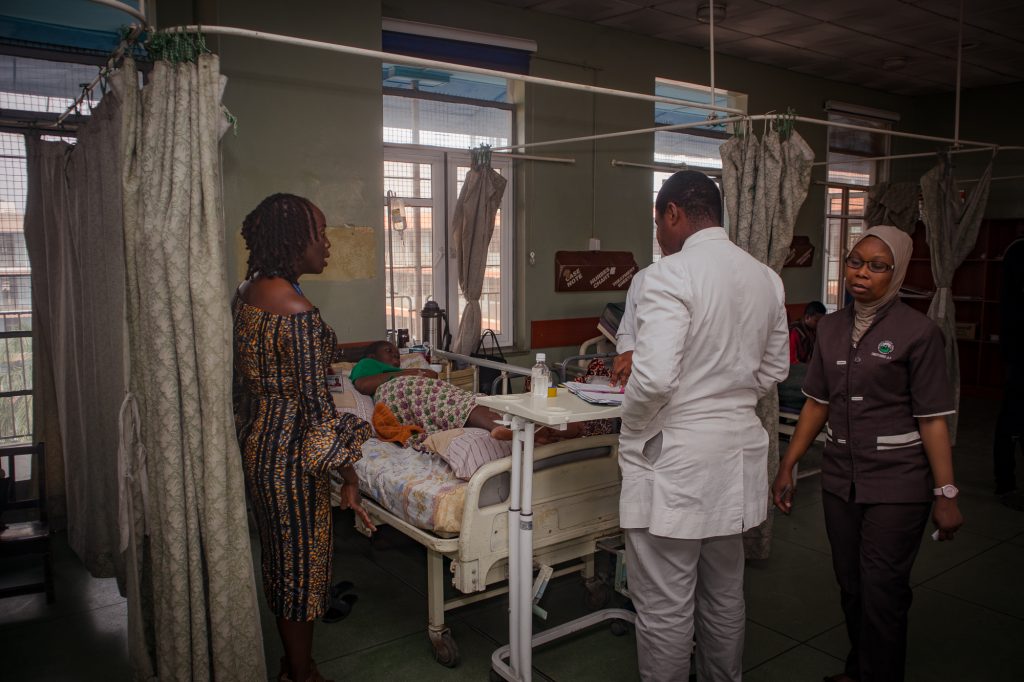
Many of the women who have taken part in the WOMAN Trials fall into these categories. They are pregnant women in low- and middle-income countries like Nigeria, Pakistan, Tanzania and Zambia. Most of them don’t have money to pay for healthcare. In the WOMAN-2 Trial specifically, the women also all had moderate to severe anaemia, already putting them at a disadvantage as they are about to embark on a potentially life-threatening – albeit one that doesn’t need to be – experience: giving birth.
The WOMAN Trials are producing the evidence needed to stop women dying in childbirth. Heavy bleeding after childbirth, or postpartum haemorrhage, is the main cause of maternal death, killing around 70,000 women every year. The WOMAN Trials are looking at the effect of the drug tranexamic acid (TXA) on bleeding and the best ways to give it.
Our work has highlighted multiple ways in which women’s basic right to health is not being upheld.
Exclusion from medical research
First, the fact that these women are being included in clinical trials for the first time highlights the fact that they are normally excluded. Some degree of caution with administering medication to pregnant women is understandable and changes in drug absorption, distribution and metabolism may require a different dose, but exclusion from clinical trials is not the answer. Most women take some form of medication in pregnancy, so these groups should absolutely be included in medical research.
A significant issue is that a lack of knowledge on the effectiveness and safety of medicines in pregnancy causes major problems when pregnant women need healthcare. The basic human right of access to healthcare is not being met, if pregnant women cannot benefit from research or scientific advancement.
Anaemia
Second, the WOMAN-2 Trial has given us an extremely important insight into the impact of anaemia on pregnancy and childbirth. Last year, we published research in the Lancet Global Health showing that pregnant women with anaemia are substantially more likely to suffer life-threatening bleeding after childbirth. The findings show the pressing need for changes in policy and practice to prioritise the treatment and prevention of anaemia in women of reproductive age.
Worldwide, half a billion women are anaemic. Anaemia is more of a risk in low- and middle-income countries where women’s nutritional needs are not necessarily being met and there are other common infections, such as malaria.
Anecdotally, we are seeing that many anaemic women give birth without even knowing they are anaemic – this is not good obstetric care. Women are not being tested for anaemia, as it is not normal practice, because it costs money and people simply cannot afford it. Not having access to a basic health service like a haemaglobin test highlights global health inequalities for the most vulnerable at their most vulnerable time.
As a matter of urgency, we need to prevent, detect and treat anaemia in women. This should be part of women’s basic right to the health services they need to ensure they and their babies are as safe as possible going into childbirth and after delivery.
Pain relief
Third, a 2022 comment in the Lancet Public Health said: “Access to pain relief medication is one of the most heinous, hidden inequities in global health.” People all over the world are suffering from avoidable pain because of a lack of access to medication that should a basic right, and this of course includes millions of pregnant women.
The chasm between what pain relief is available to women in high-income and those in low-income countries is huge. A first glance at data from the WOMAN-2 Trial – results will be published this summer – shows just that only 12% of the 15,000 women who took part in the trial received any form of pain control. Less than 1% of women had an epidural. According to data from the Care Quality Commission, 31% of women in the UK who gave birth in 2019 received an epidural.
What needs to happen
For “my health, my right” to be reflected in the care and services that pregnant women around the world can access, action needs to be taken.
We need more data: how many pregnant women are anaemic and how anaemic are they? They need to be tested and treated long before they arrive in the delivery room, for their sake and their babies’. The WOMAN Trials are contributing to this, but a lot more needs to be done.
We don’t yet know if TXA will help these vulnerable women. The WOMAN-2 Trial will provide the answer, as well as the I’M WOMAN Trial, which is starting to recruit women.
Once we know the results, we have a duty to communicate them as widely as possibly – to healthcare professionals, ministries of health, organisations like the WHO and, of course, women around the world.